What is it?
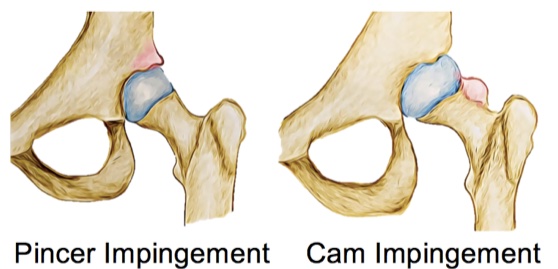
When the two surfaces of the hip joint move over each other, they usually move freely without any friction. If there is an alteration to either the socket part of the joint (the acetabulum) or the ball (the head of the femur), irritation may occur as the two surfaces move over each other. This is known as Femoroacetabular impingement (or FAI) a common disorder of the hip, characterised by pain and stiffness.
Femoroacetabular impingement can be classified as cam, pincer or mixed. A cam FAI occurs when the femoral head junction is flattened or a small bump is present. Pincer type of impingement occurs when the acetabular rim extends slightly, causing the femur to be impacted. Cam impingement is more common in men while pincer impingement is more common in women. However, most cases of FAI (about 85%) are mixed, meaning they both have cam and pincer types of impingement.
What are the symptoms?
The most common symptom of FAI is pain located in the hip or groin when resting in certain positions or with specific movements. Some patients also report pain in the back, buttock or thigh. Other symptoms include stiffness, loss of movement range (particularly of the hip), locking, clicking or a feeling that the hip is about to give way.
Activities that cause the incongruous surfaces to move over each other repeatedly are naturally the main culprits for causing symptoms. These can include prolonged sitting, twisting, sitting with crossed legs, squatting and climbing stairs can all aggravate the pain caused by femoroacetabular impingement.
What are the causes?
There are many factors that may cause an individual to develop femoroacetabular impingement including;
- Hip dysplasia or malformation during infancy/childhood
- Repetitive stress on the hip
- A femoral neck fracture that did not heal properly (malunion)
- Small bony growths around the joint called osteophytes.
- Normal anatomical variation
How can physiotherapy help?
Femoroacetabular impingement is a complex condition and researchers are still determining the best possible treatment. It is thought that untreated FAI can lead to osteoarthritis of the hip down the track and there are both surgical and non-surgical options for treatment. Conservative (non-surgical) management for FAI involves core stability training, strengthening exercises for the lower limb specifically the hip and postural balance exercises. This program aims to improve the hip’s neuromuscular function. A hydrotherapy program can also helpful as it reduces weight through the joint, making movements more comfortable. Lastly, a home exercise program is made for patients, so they can continue treatment at home. For many people, physiotherapy is enough to resolve their symptoms and prevent future problems, however others may require surgery.
With surgery, hip arthroscopy is the most common procedure for this disorder and is used to change the shape of the joint slightly so that there are no points of irritation with movement. After surgery, patients are usually referred to physiotherapy for rehabilitation.
None of the information in this article is a replacement for proper medical advice. Always see a medical professional for advice on your individual condition.